Aquamantys™
Aquamantys™ bipolar sealers use proprietary Transcollation™ technology, combining radiofrequency (RF) energy and saline to provide haemostatic sealing of soft tissue and bone without the smoke or char found in other methods.
The combination of RF energy and saline allows the device to operate at approximately 100˚C — nearly 200˚C less than traditional electrosurgical devices. By controlling bleeding, Aquamantys™ has been shown to significantly reduce the incidence of haematoma and reduce surgical time in a variety of procedures, and may reduce the need for haemostatic agents.[1-5]
1. Geller DA, Tsung A, Maheshwari V, Rutstein LA, Fung JJ, Marsh JW. Hepatic resection in 170 patients using saline-cooled radiofrequency coagulation. HPB (Oxford). 2005;7(3):208–213.
2. Marulanda GA, Ulrich SD, Seyler TM, Delanois RE, Mont MA. Reductions in blood loss with a bipolar sealer in total hip arthroplasty. Expert Rev Med Devices. 2008;5(2):125–131.
3. Ackerman SJ, Tapia CI, Baik R, Pivec R, Mont MA. Use of a bipolar sealer in total hip arthroplasty: medical resource use and costs using a hospital administrative database. Orthopedics 2014;37(5):e472–481.
4. Weeden SH, Schmidt RH, Isabell G. Haemostatic efficacy of a bipolar sealing device in minimally invasive total knee arthroplasty. J Bone Joint Surg Br Proceedings 2009; 91–B:45.
5. Clement RC, Derman PB, Graham DS, Speck RM, Flynn DN, Levin LS, Fleisher LA. Risk factors, causes, and the economic implications of unplanned readmissions following total hip arthroplasty. J Arthroplasty. 2013 Sep;28(8 Suppl):7-10.
Use in Hip Arthroplasty
Use in Knee Arthroplasty
Achieving Haemostasis
These illustrations show how Aquamantys™ bipolar sealers achieve haemostasis with heat-induced collagen shrinkage in blood vessel walls.
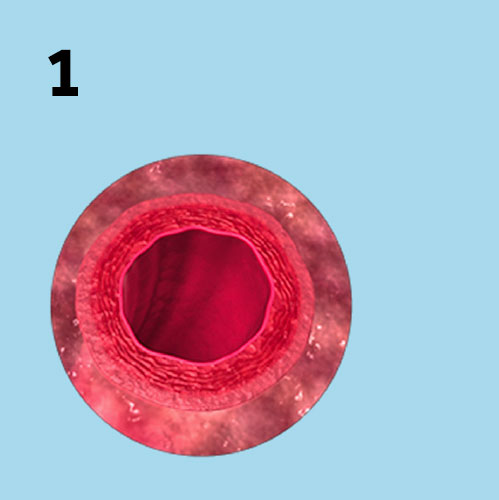
1. RF energy and saline are applied to tissue.
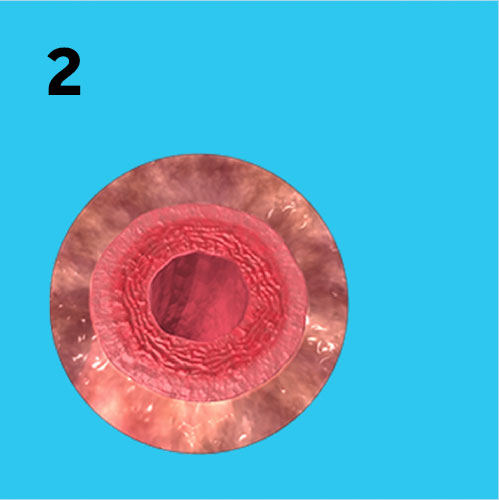
2. Heat-induced collagen shrinkage occurs.

3. Vessels <1 mm may be occluded.
Benefits
Economic
Patient
3. Ackerman SJ, Tapia CI, Baik R, Pivec R, Mont MA. Use of a bipolar sealer in total hip arthroplasty: medical resource use and costs using a hospital administrative database. Orthopedics 2014;37(5):e472–481.
4. Weeden SH, Schmidt RH, Isabell G. Haemostatic efficacy of a bipolar sealing device in minimally invasive total knee arthroplasty. J Bone Joint Surg Br Proceedings 2009; 91–B:45.
5. Clement RC, Derman PB, Graham DS, Speck RM, Flynn DN, Levin LS, Fleisher LA. Risk factors, causes, and the economic implications of unplanned readmissions following total hip arthroplasty. J Arthroplasty. 2013 Sep;28(8 Suppl):7-10.
6. Ibrahim M, Menna C, Maurizi G, et al. Impact of Transcollation technology in thoracic surgery: a retrospective study. Eur J Cardiothorac Surg. 2016;46(2):623-6.
1. Geller DA, Tsung A, Maheshwari V, Rutstein LA, Fung JJ, Marsh JW. Hepatic resection in 170 patients using saline-cooled radiofrequency coagulation. HPB (Oxford). 2005;7(3):208–213.
7. Bierbaum BE, Callaghan JJ, Galante JO, Rubash HE, Tooms RE, Welch RB. An analysis of blood management in patients having a total hip or knee arthroplasty. J Bone Joint Surg Am. 1999;81(1):2-10.
8. Suarez JC, Slotkin EM, Szubski CR, Barsoum WK, Patel PD. Prospective, Randomized Trial to Evaluate Efficacy of a Bipolar Sealer in Direct Anterior Approach Total Hip Arthroplasty. J Arthroplasty 2015;30(11):1953-8.
9. Data on file. Report 81-10-5683.
10. Procyk S. The Transcollation: Short Hospitals Stay and Accelerated Recovery in Total Hip and Knee Arthroplasties Using a Radiofrequency Bipolar Sealer - an Innovative Approach in the Conceptualization of the Surgical Gesture. Natl Acad of Surg 2015:15(2):87-97.
2. Marulanda GA, Ulrich SD, Seyler TM, Delanois RE, Mont MA. Reductions in blood loss with a bipolar sealer in total hip arthroplasty. Expert Rev Med Devices. 2008;5(2):125–131.

MBS MALLEABLE BIPOLAR SEALER WITH LIGHT
23-301-1
Malleable shaft and built-in light allow access to hard-to-reach anatomy and provide illumination during surgery.

6.0 BIPOLAR SEALER
23-112-1
Large-sized electrodes provide haemostatic sealing of soft tissue and bone.

2.3 BIPOLAR SEALER
23-113-1
Medium-sized electrodes provide more precise application for haemostatic sealing.

MINI EVS 3.4 EPIDURAL VEIN SEALER
23-314-1
3.4mm tip size for small epidural access points, and insulated shaft enables simultaneous retraction and electrode use near sensitive tissue such as dura and nerve roots.

EVS EPIDURAL VEIN SEALER
23-121-1
Insulated shaft enables electrode use near sensitive tissue such as dura and nerve roots.

9.5XL BIPOLAR SEALER
23-313-1
Cone-shaped electrodes aid in blunt dissection and haemostatic sealing.

SBS 5.0 SHEATHED BIPOLAR SEALER
23-312-1
Retractable sheath enables simultaneous retraction and electrode use near sensitive tissue such as dura and nerve roots (sheath closed), and haemostatic sealing of soft tissue and bone (sheath open).

ENDO VS 8.7R VATS BIPOLAR SEALER
23-320-1
Rounded electrodes allow for broad plane haemostasis on chest wall.

ENDO DBS 8.7 DISSECTING BIPOLAR SEALER
23-317-1
Laparoscopic length enables minimally-invasive procedures, with cone- shaped electrodes to aid in blunt dissection.
Revolution Surgical Pty Ltd
5/14-16 Crescent Street, Rozelle NSW 2039 AU
ABN: 63 165 643 434
© 2018-2024 Revolution Surgical
